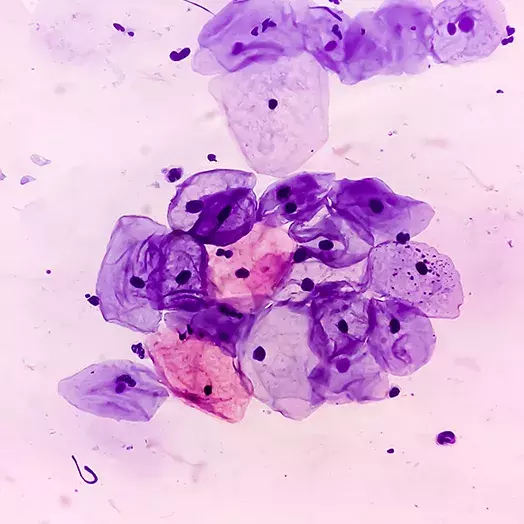
Could artificial intelligence in a “smart tampon” detect cervical cancer?
Editor’s note: January is Cervical Cancer Awareness Month. We are re-sharing this story, initially published in September 2022, to underscore the potential for artificial intelligence to save lives while closing the gaps in equitable health care.
Four students might have just come up with an idea that could save thousands of lives a year in the U.S. while cutting down on health care costs and inequities.
The Johns Hopkins Carey Business School alumni —Charlie Acosta, Hayley Hoaglund, Tomas Delia, and Madeleine Howard—developed the “smart tampon” innovation in their artificial intelligence course lab as part of their full-time MBA program. It combines what they learned about economic forces, business applications, and mathematical and computational foundations to come up with the AI application.
“COVID-19 has forced the field of health care to be more innovative than it has ever been,” said Hoaglund. “The US has the highest spending on health care in the world, so if we can re-think how we deliver essential services, there is a tremendous opportunity for cost savings and to increase access to care.”
How it could work
Cervical cancer is typically detected through a Pap smear, which is a test that scrapes the surface of the cervix to collect cells for examination and detection of unusual growth. Medical experts advise that the average woman between ages 21 and 65 have this test every three years. But between work and wages lost for the appointment, the potential costs of the visit, and the discomfort and anxiety it can cause, many women forego the screening, allowing a disease that’s highly treatable in early stages to advance before detection.
As conceived by the Carey group, the “smart tampon” would be inserted as a normal tampon would, though not during menstruation and only for the time it takes to gather data. At its top, a highly sensitive camera would take images of the cervix and feed them into AI-integrated software for analysis. This would be connected to an app, to which the provider and the patient would have access. A simple red light would tell the provider there could be an irregularity, and would prompt the user to seek medical care. A green light would indicate normal cervical health.
If the invention attracts investors who want to help it get to market, the student researchers believe it could be prescribed by a provider once every three years, and be covered by insurance.
What to Read Next

career outcomes
A joint venture: MBA alums co-found stealth startup to tackle the gaps in patient equityWhy AI?
The smart tampon project was one of 16 projects Carey students in the full-time MBA program created as part of their required AI course. In addition to deep concepts of AI, the Carey course introduces students to reinforcement learning, a type of artificial intelligence that, rather than learning from data, self-teaches by exploring and acting on what it learns. Beyond the business element of AI, the course also addresses AI’s limitations, and how it can contribute to better inclusivity, equity, and fairness in society.
“To the best of my knowledge, Carey is likely the first business school in the United States to require every full-time MBA student to take an AI course,” said Carey Professor Tinglong Dai, PhD, an expert in AI who designed and teaches the course. “This is a game-changing move that will have far-reaching implications not only for Carey and Johns Hopkins, but also for the future of business education.”
Dai said “deep learning” has taken center stage the AI field in the last decade, helping to expand the landscape of its impact.
“The future of business lies in the synthesis of human and non-human intelligence,” he said. “A future-proof business leader must be acutely aware of the inner workings of AI and its limitations. Our students will be uniquely prepared to be those leaders.”


